Question 11#
You are covering the general medical service one evening when contacted by the nursing staff about a “critical” lab test on a patient. The patient in question is a 62-yearold man who was admitted to the hospital with community-acquired pneumonia. His comorbidities include diabetes mellitus and chronic kidney disease. The patient had a scheduled chemistry panel, which showed potassium of 6.5 mEq/L. You immediately order an EKG.
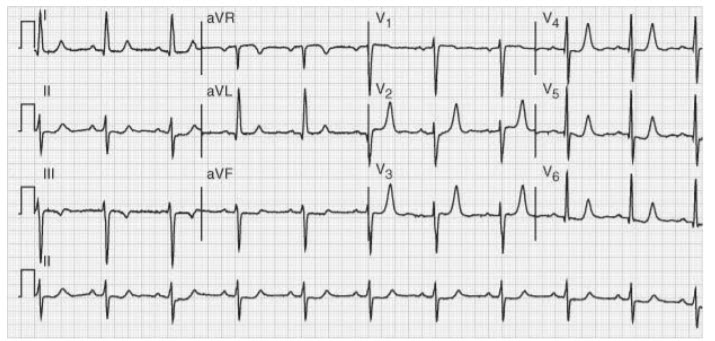
What is the next best step in management of this patient’s hyperkalemia?
A. Administer IV calcium gluconateB. Administer oral sodium polystyrene sulfonate (Kayexalate)
C. Administer subcutaneous insulin
D. Administer IV bicarbonate
E. Repeat the serum potassium
Correct Answer is A
Comment:
The patient has electrocardiographic changes of hyperkalemia and is at risk of rapid deterioration. The usual EKG findings seen with hyperkalemia (in order of progressive risk of arrhythmia) include peaked T waves, prolongation of the PR interval, widening of the QRS segment, and loss of P waves. Progressive QRS widening with subsequent merger with the T wave produces a sine wave that precedes the terminal ventricular fibrillation or asystole. Management of hyperkalemia frequently requires several interventions based on the rapidity of onset and duration of effect of the therapy. When there is EKG evidence of hyperkalemia, immediate administration of IV calcium to stabilize the cellular membrane is indicated. Acting almost immediately, the stabilizing effect of calcium will last 30 to 60 minutes, allowing time for other corrective measures to be taken. The calcium dose may be repeated if initial dosing does not reverse EKG changes, or if the implementation of other corrective measures is delayed. Following initial membrane stabilization with calcium, attention is then turned to other fast-acting therapies to decrease the serum potassium concentration. Insulin moves potassium into cells via insulin-dependent K + /glucose cotransporter, but for rapid effect the insulin should be given intravenously. Unless the patient is hyperglycemic, IV glucose is also given to prevent hypoglycemia. The usual dose is 10 units of insulin and 25 g of IV glucose (one ampule of D50). Beta agonists can also be used to drive potassium into cells. Bicarbonate therapy will cause the potassium to shift intracellularly via H + /K + ion exchange as the body attempts to stabilize the pH. Given the risks associated with bicarbonate therapy, this therapy is usually reserved for patients who are significantly acidotic and are able to be effectively ventilated. Each of these therapies has relatively rapid onset of action, but none changes the total body potassium content, and therefore they are bridge therapies until therapies to actually deplete potassium stores can be implemented. Loop diuretics and sodium polystyrene sulfonate (a potassium binder) will both reduce potassium stores in the body. Hemodialysis is utilized in refractory cases, or in chronic kidney disease patients who already have dialysis access. It is very reasonable to repeat the potassium if you feel that it may be a lab error (answer e). In the presence of electrocardiographic changes suggestive of severe hyperkalemia, however, you should “treat first and ask questions later.”