Question 4#
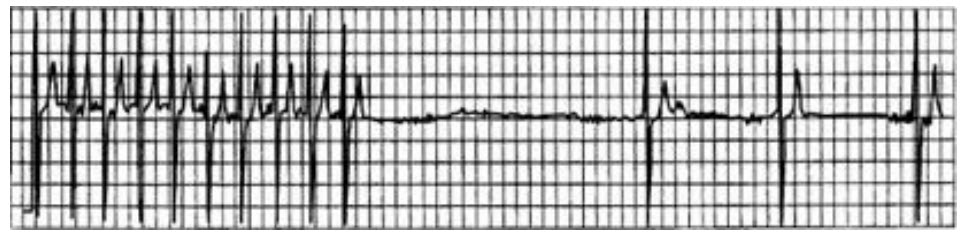
An 82-year-old white woman is admitted to the hospital for observation after presenting to the emergency department with dizziness. After being placed on a cardiac monitor in the ER, the rhythm strip below was recorded. There is no past history of cardiac disease, diabetes, or hypertension. With prompting, the patient discloses several prior episodes of transient dizziness and one episode of brief syncope in the past. Physical examination is unremarkable. Which of the following is the best plan of care?
B. Reassurance. The patient may not drive until she is symptom free, but otherwise no direct therapy is needed
C. Nuclear cardiac stress testing; treatment depending on results
D. Begin therapy with aspirin
E. Arrange placement of a permanent pacemaker
Correct Answer is E
Comment:
The patient in question has symptomatic tachycardia-bradycardia syndrome. Sinus node automaticity is suppressed by the tachyarrhythmia and results in a prolonged sinus pause following termination of the tachycardia. The patient in this case is symptomatic, and pacemaker placement is warranted; reassurance would put the patient at risk of further syncopal episodes and bodily harm from fall or accident. Although a pacemaker will prevent bradycardia, it does not prevent tachycardia. The patient may need medication to prevent tachycardia if she continues to be symptomatic after pacemaker placement. It is unlikely that any positive findings on a stress test could be correlated with her ECG findings. The tachy-brady syndrome does increase the patient’s risk of cardioembolic event, and anticoagulation should be considered. Aspirin, however, is not an appropriate agent to prevent cardiogenic embolism.