Question 1#
A 54-year-old man presents to the hospital with a 3-day history of severe nausea, vomiting, and diarrhea. He has been unable to keep down substantial solids or liquids over the past few days and has become progressively weak. He also endorses subjective fevers and occasional abdominal pain. The patient’s medical history is significant for hypertension and chronic low back pain, for which he takes lisinopril and ibuprofen. He has a 4-year-old child that he picks up from daycare who has also had diarrhea. On examination, the patient is tachycardic with a blood pressure of 104/84 mmHg. He appears weak with dry mucus membranes. Routine laboratory values are drawn, which show a blood urea nitrogen (BUN) and creatinine of 40 mg/dL and 2.1 mg/dL, respectively. He denies any history of renal disease.
Of the following options, what would be most helpful in determining the etiology of this patient’s renal failure?
A. Urine dipstickB. Urine sodium
C. Fractional excretion of sodium (FENa)
D. Renal ultrasound
E. No further workup is necessary
Correct Answer is C
Comment:
Fractional excretion of sodium (FENa). Acute kidney injury (AKI) was defined by the Acute Kidney Injury Network (AKIN) as an abrupt rise (within 48 hours) in serum creatinine by ≥0.3 mg/dL from baseline, a ≥50% increase in serum creatinine from baseline, or oliguria of <0.5 cc/kg/h for >6 hours. Once AKI is recognized, the next step in diagnosis is determining whether the etiology is prerenal, intrinsic renal, or postrenal (Figure below). These terms reflect the perceived sight of pathology; prerenal AKI is caused by decreased blood flow to the kidneys, intrinsic renal AKI is caused by direct damage to the kidney parenchyma (i.e., to the renal vasculature, tubules/interstitium, or glomeruli), and postrenal AKI is caused by an obstruction in the urinary tract leading away from the kidneys.
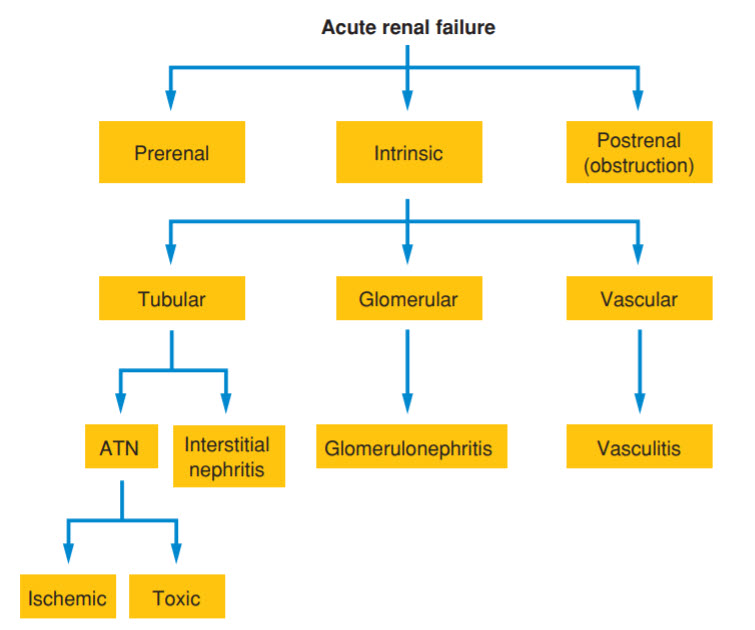
The patient in this question is hypovolemic (tachycardia, decreased pulse pressure, and dry mucus membranes) from acute gastroenteritis that he likely acquired from his child. In response to hypovolemia, the renal arterioles vasoconstrict, decreasing blood flow to the kidneys and decreasing the glomerular filtration rate (GFR). Prerenal AKI is a result of ischemia from poor perfusion; however, it can progress to acute tubular necrosis (ATN), which is a form of intrinsic renal AKI. Besides hypovolemia, his daily NSAID may also be contributing to the AKI since NSAIDs cause renal vasoconstriction. The combination of an NSAID and an ACE inhibitor can worsen a more mild renal failure. One of the best tests for differentiating between prerenal AKI and ATN is the FENa. In prerenal AKI, sodium is reabsorbed in an attempt to maintain circulating blood volume, and therefore there will be little sodium in the urine. (B) Although this is often reflected by the urine sodium, this value is affected by renal water handling and urine output. FENa is a better test, since it only measures the fraction of sodium excretion and is not affected by urine output. In general, low FENa values indicate prerenal AKI and high values indicate intrinsic renal AKI (tubular damage leads to salt wasting). The FENa will be <1% in prerenal AKI and >2% in ATN. (Note: FENa should not be used in the setting of diuretics, but the fractional excretion of urea may be used instead.)
(A) A urine dipstick is a helpful screening tool for things like proteinuria or infection, but it will not help to differentiate between prerenal and intrinsic renal AKI. (D) A renal ultrasound is helpful in excluding postrenal AKI, which is not suspected in this case (sudden urinary tract obstruction is unlikely given the patient’s history of vomiting and diarrhea). (E) The diagnosis of prerenal AKI versus ATN cannot be made by history alone.