Question 1#
A 49-year-old female is admitted to the medical intensive care unit with sepsis due to pyelonephritis and acute kidney injury. Prior urinary tract infections have been due to extended-spectrum Blactamase Escherichia coli. Her initial pertinent lab values include creatinine 1.8 mg/dL, BUN 32 mg/dL, WBC 22.4 × 10 9 /L with elevated band percentage (24%). She was resuscitated with 6 L of IV fluids and started on norepinephrine to maintain a mean arterial pressure of 65. Empiric antibiotic therapy was started with imipenem and vancomycin. Over the course of 48 hours she has improvement in her lab values and vitals and was weaned from vasoactive medications. Despite improvement in the above, she has had ongoing alteration in her level of consciousness. She underwent a prolonged EEG monitoring (see figure tbelow).
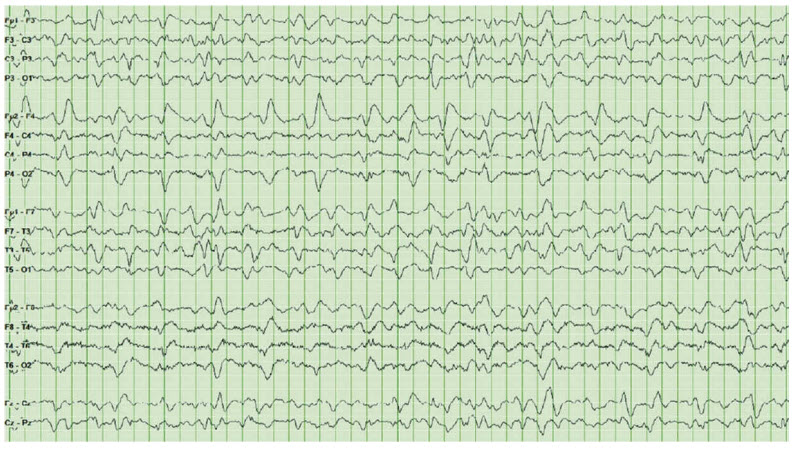
Standard 10 to 20 electrode placement. This is a standard “double banana” montage with left over right. EEG demonstrates broad, generalized periodic discharges right greater than left hemispheric involvement.
What is the next best step in management?
A. Change of imipenem to different antibiotic given ongoing seizuresB. Continue with supportive care and no change to medications
C. Initiation of antiepileptic medication—levetiracetam 500 mg twice a day
D. Benzodiazepine trial—lorazepam 1 mg IV once
Correct Answer is D
Comment:
Correct Answer: D
The EEG above demonstrates triphasic waves. The triphasic wave has a high-amplitude (>70 microV), positive transient followed by a negative deflection with an anterior-posterior gradient and anterior-posterior delay. Triphasic waves were initially described in hepatic encephalopathy but have been described in multiple metabolic derangements, and they can be associated with nonconvulsive seizures. Treatment of triphasic waves with benzodiazepine will result in improvement in the discharges, but it may not change the clinical picture of the patient. A trial of benzodiazepine might help in the diagnosis of nonconvulsive status. A positive benzodiazepine test if there is resolution of potentially ictal EEG pattern and improvement in clinical state or appearance of previously absent normal EEG pattern. If there is demonstration of the above, then treatment with an AED would be appropriate. Imipenem and other carbapenem medications have been associated with increased risk of seizures; with imipenem use, 4/1000 patients have seized.
References:
- Brigo F, Storti M. Triphasic waves. Am J Electroneurodiagnostic Technol. 2011;51:16-25.
- Fountain NB, Waldman WA. Effects of benzodiazepines on triphasic waves: implications for non-convulsive status epilepticus. J Clin Neurophysiol. 2001;18:345-352.
- Jirsch J, Hirsch LJ. Nonconvulsive seizures: developing a rational approach to the diagnosis and management in the critically ill population. Clin Neurophysiol. 2007;118:1660-1670.
- Cannon JP, Lee TA, Clark NM, et al. The risk of seizures among the carbapenems: a meta-analysis. J Antimicrob Chemother. 2014;69:2043- 2055.