Question 3#
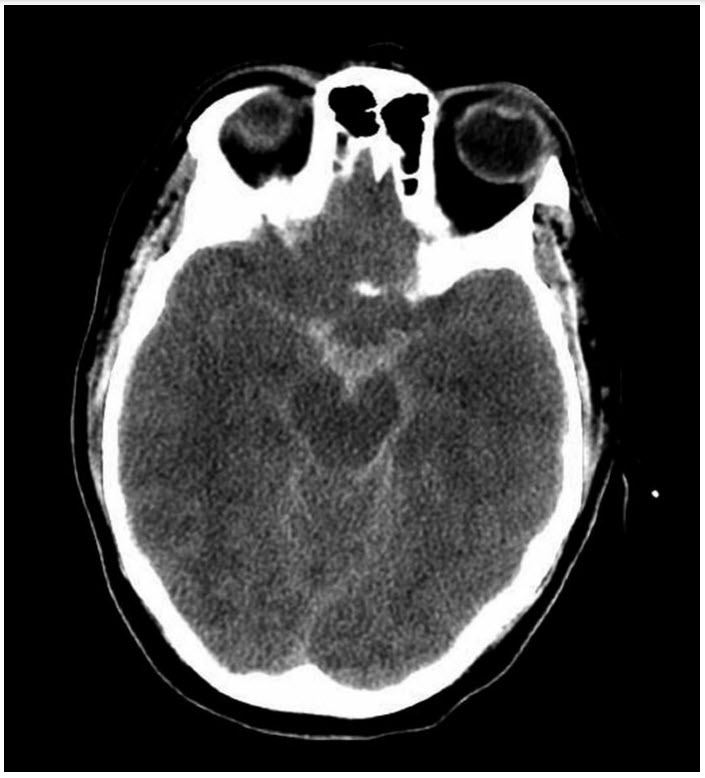
A 45-year-old woman, who is an active smoker and has history of untreated hypertension, presented following a sudden “thunderclap” headache. Head CT revealed (see figure below) subarachnoid hemorrhage of an anterior communicating artery aneurysm. She underwent successful endovascular coiling of the aneurysm, and an external ventricular drain was placed for hydrocephalus. Five days after presentation, she acutely became somnolent.
Vital signs are
- T 37.4
- HR 94
- R 24
- BP 124/75 (MAP 91)
- O2 saturation 95% on room air
On examination she is somnolent but easily arousable and follows simple commands with all four extremities, but there is a clear drift of the right hand and leg.
What is the most appropriate next step in management?
A. Administer stat IV LevetiracetamB. Bolus 1 liter of fluid
C. Consult interventional radiology for stat angioplasty
D. Administer empiric IV Vancomycin and Ceftriaxone in meningitis doses
Correct Answer is B
Comment:
Correct Answer: B
This patient has a classic presentation of symptomatic cerebral vasospasm and delayed cerebral ischemia after sub-arachnoid hemorrhage. She has several risk factors for vasospasm, including: sex, smoking history, and the blood pattern on the head CT (blood in the cistern and the presence of intraventricular blood). The highest incidence of vasospasm occurs between post-bleed days 4 to 10 (although it can occur up to three weeks post bleed). Although angioplasty is a definitive treatment for vasospasm, the first bedside intervention should be fluid administration to increase the mean arterial pressure (MAP) to improve cerebral perfusion. The description is not suggestive of a seizure and therefore choice A is incorrect. The description also does not suggest a new infection, and therefore Answer D is incorrect.
Reference:
- Francoeur CL, Mayer SA. Management of delayed cerebral ischemia after subarachnoid hemorrhage. Crit Care. 2016;20(91):277.